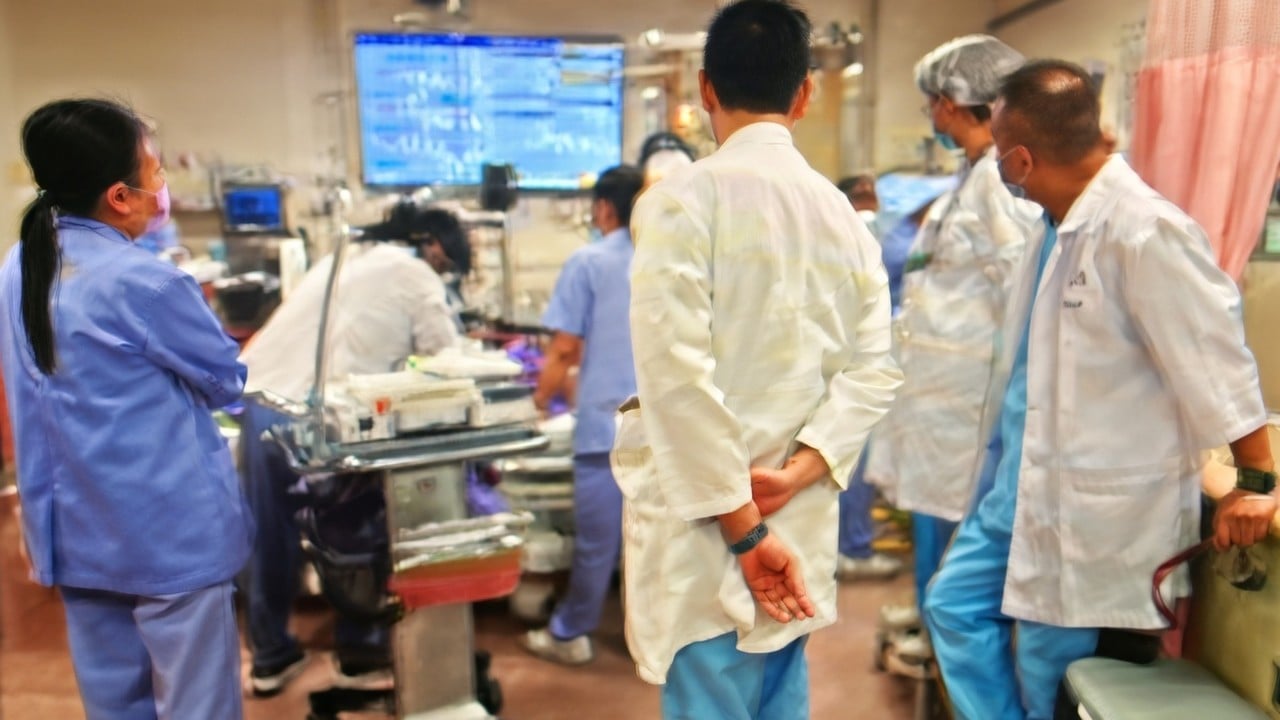
Hospital administrators are chasing a ghost.
The recent investigation by the Hospital Authority into a doctor’s social media post is being framed as a breach of patient privacy. That is a convenient, surface-level lie. It allows bureaucrats to tick a compliance box while ignoring the actual rot in modern medicine: the total collapse of the professional boundary and the commodification of the white coat.
When a doctor posts a "day in the life" video or shares a clinical anecdote for likes, they aren't just risking a HIPAA violation. They are dismantling the clinical distance required to actually save lives.
Stop asking if the patient’s face was blurred. Start asking why the doctor felt the need to broadcast from the theater of trauma in the first place.
The Compliance Fallacy
The "lazy consensus" among hospital PR teams is that privacy training solves the problem. It doesn't. You can give a surgeon a thousand hours of data-governance seminars, and they will still find a way to post a "relatable" selfie with a gurney in the background.
The issue isn't a lack of rules. The issue is a fundamental misunderstanding of what a hospital is.
In the industry, we call this the "Disneyfication" of healthcare. Hospitals are being treated like content goldmines. Every patient interaction is viewed by younger practitioners not as a sacred duty, but as a potential "story" for their personal brand.
I have seen departments spend $200,000 on digital ethics consultants only to have a resident leak a "funny" patient quote on a private Discord ten minutes later. The rules are theater. The culture is the problem.
The Nuance Everyone Misses
Privacy isn't a binary state. It’s an ecosystem.
- De-identification is a Myth: With modern metadata and "mosaic" identification, you don't need a name to identify a patient. A specific rare condition, a timestamp, and a hospital logo are enough for any bored internet sleuth to dox a victim.
- The Consent Paradox: Even if a patient "consents" to be in a video, the power dynamic is so skewed that the consent is ethically void. A patient in a hospital gown is in no position to tell their surgeon "no" when a ring light is involved.
- The Ego Tax: Every second a clinician spends framing a shot is a second they aren't thinking about the $K^{+}$ levels in Room 402.
The False Promise of the Humanized Doctor
The common defense for these social media posts is that they "humanize" the profession. This is a catastrophic error in judgment.
Patients do not go to the ER because they want a friend. They go because they want an expert. When you see your cardiologist doing a TikTok dance or complaining about "difficult patients" for clout, that expert-client relationship is shattered.
We are trading Authority for Relatability. It’s a bad trade.
The Brutal Reality of Digital Permanence
Imagine a scenario where a doctor posts a redacted case study to "educate" their followers. It’s educational, right?
Wrong. It’s vanity.
True medical education happens in peer-reviewed journals and closed Grand Rounds. Social media "education" is almost always a performance of intelligence rather than a transfer of knowledge.
When a Hospital Authority "investigates" a post, they focus on the specific pixels. They should be focusing on the intent. If the intent was to gain followers using the suffering of others as a backdrop, the doctor has already failed the most basic tenet of the Hippocratic Oath.
The Internal Cost of "Going Viral"
I’ve watched careers vanish because of one "clever" caption. The tragedy isn't the lost job; it's the lost trust. When a community realizes their local hospital is a backdrop for Instagram influencers, they stop being honest with their providers. They withhold information. They fear being the next "crazy patient story."
The data on medical trust is clear. According to recent longitudinal studies on patient-provider relationships, the perception of professional detachment is actually a predictor of patient satisfaction in high-stakes environments. We want our pilots and our surgeons to be slightly robotic. We want them focused on the mission, not the engagement metrics.
Fix the Culture, Not the Captions
If you want to stop the "privacy concerns," stop rewarding the behavior.
- Ban Personal Devices in Clinical Areas: This was the standard twenty years ago. It should be the standard now. If it isn't hospital-issued and encrypted, it doesn't belong in the ward.
- Zero-Tolerance for Patient Content: Not "blurred faces." Not "de-identified stories." Zero. If a patient’s existence is used to bolster a doctor’s social media standing, that doctor should be out of a job.
- Kill the "Brand": Hospitals need to remind staff that they are employees, not independent content creators.
The Hospital Authority shouldn't be "investigating." They should be exiling.
The Question You Aren't Asking
"How do we protect patient privacy online?" is the wrong question.
The real question is: "How did we allow the most serious profession on earth to become a sub-genre of lifestyle vlogging?"
The "privacy breach" is just a symptom of a deeper, more dangerous narcissism. If we don't treat the narcissism, the privacy leaks will continue until the very idea of a "private" medical record is a joke of the past.
Healthcare isn't a stage. The patient isn't a prop.
Put the phone down and do your job.